We all know someone who has taken a day off work to get a colonoscopy, along with the usual jokes about staying near a bathroom during the cleanse and finding a trusted friend to chauffeur them after the procedure. All joking aside, colonoscopies save lives.
The second-leading cause of cancer fatalities in the United States is due to colorectal cancer. Regular colonoscopy screening discovers colorectal cancer and polyps that, left untreated, may lead to cancer. In a recent journal, the American Cancer Society recommends that people of average risk be screened with a colonoscopy beginning at age 45, instead of 50, due to an increased risk of colorectal cancer in younger age groups.
Discussing Your Risk Factors
The age of the first colonoscopy or the frequency needed for testing depends on a person’s family history, physical condition, and personal health risk factors.
Risks include:
- Your own history of colon cancer or pre-cancerous polyps
- Family history of colon cancer, especially in your immediate family
- Having a gene for the syndrome that leads to hereditary colon cancer
- History of ulcerative colitis or Crohn’s disease (inflammatory bowel disease)
- Ultimately, the decision for when to have the first colonoscopy rests with you and your doctor.
Colonoscopy
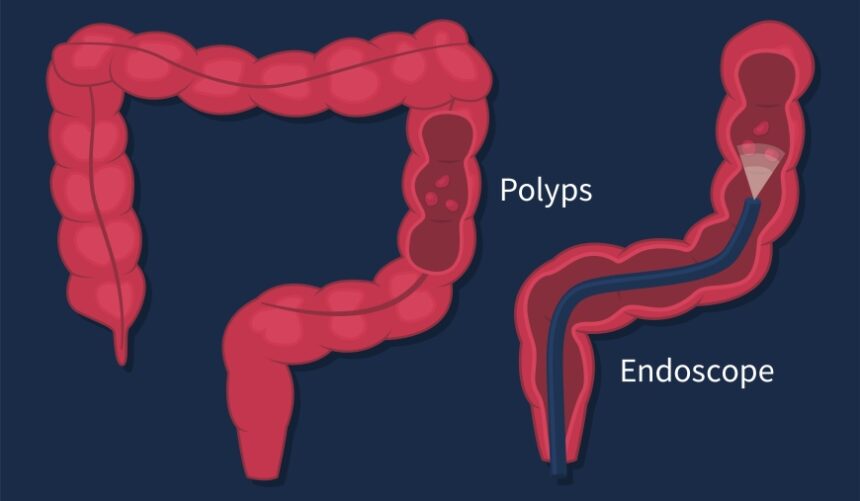
A colonoscopy is the most thorough screening exam to both detect cancer and look for pre-cancerous polyps. It is performed following a thorough preparation regimen, including avoiding solids the day before the exam and using laxatives or enemas to empty the colon. Following light sedation, a flexible tube with a tiny video camera on the end is inserted into the rectum so the doctor can view the colon and look for changes or abnormalities. Due to the sedation, a patient cannot drive themselves, and their driver must also remain in the waiting room during the procedure. The colonoscopy is usually repeated about every ten years—depending on any results found by the doctor during the exam.
For those reluctant to have a colonoscopy, other exams perform similar, although less thorough, screenings.
Other tests include:
Fecal immunochemical test (FIT)—This is a lab test that checks stool samples for hidden blood. Sample collection is done at home, and no prep regimen or sedation is needed. The test may not detect all polyps and cancers. Additional tests may be prescribed if needed to confirm results. It is usually repeated annually.
FIT- DNA Cologuard—This combines the FIT, which detects blood in the stool, with a test to detect abnormal DNA associated with colon cancer or colon polyps. Tests are repeated every three years.
Flexible sigmoidoscopy—With this exam, no sedation is needed, and bowel cleansing is used, although it is less extensive than a colonoscopy. Only the lower colon and rectum are viewed using a tiny video camera on the end of a thin, flexible tube. The upper colon isn’t examined, so any abnormalities there won’t be discovered. This procedure is repeated about every five years.
Blood DNA test—This lab test analyzes blood for an altered gene called SEPT9.
Talk to your doctor and discuss colon cancer screening options, as well as your own and your family’s medical history. Early detection is the key to treating colon cancer at its earliest stage.